By Rachel Bacon, MPH, Project Manager
The fifth International Conference on Family Planning (ICFP) is taking place this week in Kigali, Rwanda. The Conference co-hosts this year are the Bill & Melinda Gates Institute for Population and Reproductive Health and the Ministry of Health of the Republic of Rwanda. The conference theme is “investing for a lifetime of returns.”
“Lifetime of returns” refers to the well-established benefits of interventions that fall under the “family planning” rubric, including both pharmaceutical (birth control, treatment and control of sexually transmitted infections), and behavioral (natural family planning, birth spacing education, safe sex practices, etc.) categories. “Investing” evokes the notion of choosing wisely and methodically. That makes sense, for even though much spending on family planning generates substantial benefits, the reality is that health resources for low and middle income countries are extremely limited. How, then, can we go about wisely “investing” in family planning? What criteria should we use to identify the “best” investments? How do we transparently convey our findings and make a compelling case for family planning?
In the early part of this decade, I spent several years working with a Cameroonian faith-based healthcare organization and spent some time in-country collecting qualitative data on local preferences and practices for reproductive health. I am now a long way from Cameroon, but my present work is closely related. A major initiative at our Center, funded by the Bill and Melinda Gates Foundation, is the development and maintenance of an online, free-to-the-public registry. The Tufts Medical Center Global Health Cost-Effectiveness Analysis Registry catalogs published studies that measure the “bang for the buck” for a wide range of public health interventions.
In technical terms, “bang for the buck” is measured in terms of “dollars spent per disability-adjusted life year averted (DALY)”. A DALY is a measure of both lost life and diminished quality of life. For example, extending life expectancy by one year in good health averts a full disability-adjusted life year, or “DALY”. Avoiding a year of diminished function or substantial pain may avert one quarter of a DALY. The cost to avert one DALY for any particular intervention is referred to as the intervention’s “cost-effectiveness ratio”. Low ratios are more favorable – they mean we have averted DALYs at relatively low cost.
The catalog of cost-per-DALY-averted ratios in the Global Health Cost-Effectiveness Analysis Registry is a useful tool for methodically identifying the “best buys” (and “less favorable buys”) when it comes to investing in global health, including interventions that support family planning.
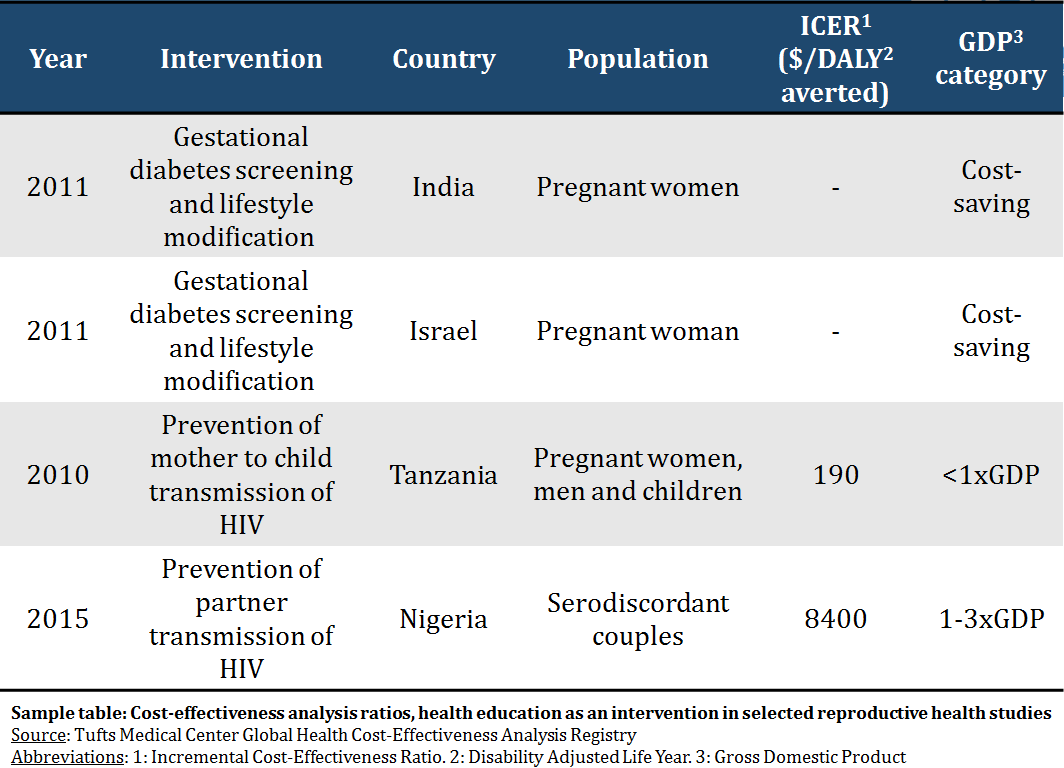
Below is a list of ratios based on health education-related reproductive health studies catalogued in the Registry. You can see that all of these interventions focus on health education and behavior change, and their cost-effectiveness ratios (far right column) range from “cost-saving” (meaning that compared to the standard of care, they reduce costs and avert more DALYs) to a per-DALY-averted cost as high as 1 and 3 times per capita gross domestic product (GDP) for the country where they are or will be implemented.
There is no “one-sized-fits all” approach to using cost-effectiveness data to justify budget expenditures, let alone a definitive silver bullet to secure funding for all programs or diseases. But with information like this, family planning advocacy groups can arm themselves with cost-effectiveness data and other information (such as local context-specific evidence: end-user demand, scientific effectiveness, multisectoral benefits, etc.) to build a case in the face of opportunity cost concerns, political pressure, demand-side constraints, or donor restrictions. When we invest in cost-effective family planning interventions, we in turn support the argument that these smart investments fulfill the promise of a “lifetime of returns.”
